Examining a patient’s brain after death may seem redundant, but it’s a central part of understanding brain diseases such as dementia. Neuroscientist Mo Costandi explains how researchers dissect brains, and why donated brains are essential in the search for treatments and cures for neurological conditions.
For a neuroscientist, there are few things as awe-inspiring as holding a human brain. This lump of flesh, roughly the size of two clenched fists and weighing about 1.5 kg, not only stored a lifetime of memories, but generated its owner’s thoughts, emotions and all their other conscious experiences.
To hold a brain is to hold the essence of the person.
We dissect brains for two main reasons. Medical students will dissect a brain, or at least watch a brain dissection, during their training, in order to learn neuroanatomy, the study of the structure and functions of the brain and nervous system. Neuropathologists may dissect a brain to determine a person’s cause of death, and to gain a better understanding of what certain diseases do to this delicate organ.

A neuropathologist begins the dissection on a donated brain at the Department of Brain Sciences, Imperial College London. This research investigates the effects on brain tissue caused by Parkinson’s disease and multiple sclerosis.
When the brain is removed from the skull and the membranes that cover it (the meninges) have been peeled off, the cerebral cortex becomes visible. The cortex (meaning ‘bark’ in Latin) is the largest part of the brain, and is characterised by the many folds and deep grooves that help us get our bearings and identify some of the main structures.
The most prominent groove is the longitudinal fissure, which runs down the centre of the brain and separates the left and right hemispheres. Another prominent groove is the central sulcus, which runs downwards from the midline, separating the frontal lobe in front of it from the parietal lobe behind it. This runs down to the lateral fissure, which separates the frontal and parietal lobes from the temporal lobe.
Gross neuroanatomy
Neuroanatomy includes the microscopic study of tissue and cells of the brain and nervous system as well as the whole brain. The study of the brain at the visible level is called gross neuroanatomy.

After removing the blood vessels at the base of the brain, the rest of the brain is cut in half along the coronal plane. One half is then placed on a cutting block and divided into precise coronal slices.
In the mid-19th century, behavioural neurologists made important discoveries just by looking at the surface of the brain. Paul Broca, the best known of them, treated two stroke patients who had lost the ability to speak. When they died, he examined their brains and noticed that they were both damaged in the same region, towards the back of the left frontal lobe. We now know that Broca’s area is a part of the motor cortex and controls the muscles in the mouth that are responsible for producing speech.
At around the same time, Carl Wernicke worked with stroke patients who had lost the ability to understand spoken language. These patients had in common damage to another region located near the back of the left temporal lobe, now known as Wernicke’s area, which is part of the brain circuit that processes sound information.
Looking at the whole brain can provide other clues. For example, the appearance of the outer membranes can show signs of meningitis and other infections; shrinkage of the brain is indicative of Alzheimer’s disease; and the condition of the blood vessels at the base of the brain can reveal hardening of the arteries due to a high-fat diet or lack of exercise.
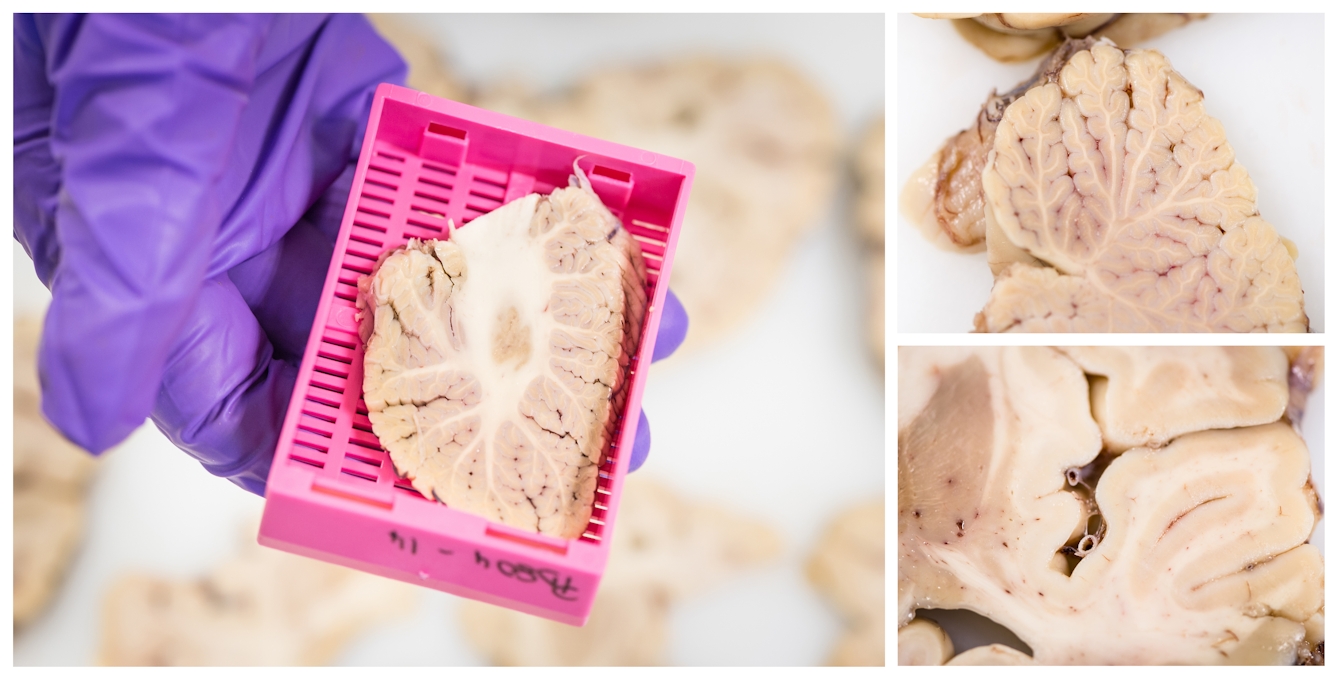
The coronal slices are placed out onto a larger cutting board where a selection of 25 samples are removed for neuropathological diagnosis.
Dissecting the brain can reveal various pathologies, or signs of disease, in greater detail. Typically, the first step of a brain dissection involves turning the brain upside down and removing the brainstem and cerebellum. These can then be examined separately to identify the characteristic hallmarks of diseases such as Parkinson’s disease.
The rest of the brain is then cut across the middle with what looks like a large bread knife, and then a series of 5 mm-thick slices, or cross-sections, are cut, with slices from one half moving progressively forward, and slices from the other moving towards the back.
Hallmarks of brain disease
Looking at these slices, it becomes immediately apparent that the brain consists of two different types of tissue. At the outer edges of the slices is the wrinkled cerebral cortex, which contains nerve-cell bodies, and has a light grey colour.

The sections of brain are protected by a paper sheet between the stages of the dissection process.
Beneath the cortex lie larger areas of lighter tissue, made up of bundles of nerve fibres connecting different brain regions to one another. These fibres are enveloped in a fatty material called myelin, which appears white in colour – hence this tissue is often referred to as “white matter”. The largest of these bundles is the corpus callosum, which contains approximately 100 million fibres connecting the left and right hemispheres, and is visible in all cross-sections except those nearest the front and back of the brain.
The devastating effects of neurological disease only add to the sense of awe neuroscientists feel when they examine the brain.
Also visible in many sections are the cerebral ventricles, a series of interconnected cavities that contain cerebrospinal fluid. The appearance of the ventricles can also provide clues about pathology; for example, the brain shrinkage that occurs in Alzheimer’s disease is associated with enlargement of the ventricles.

The samples taken are collected by the laboratory technicians for processing and embedding in wax. They are then sliced using a microtome into very thin sections (5–10 microns), which are mounted on microscope slides, ready to be stained with histological dyes and antibodies.
Alzheimer’s disease and other forms of dementia can be inferred from behaviour and memory tests, but a definitive physical diagnosis can only be made during a post-mortem neuropathological examination performed on a smaller piece of cortex taken from a cross-section. Viewed under the microscope, tissue from the brain of an Alzheimer’s patient will exhibit structures called plaques and tangles, the pathological hallmarks of the disease.
Examination of the brainstem can also reveal the hallmarks of Parkinson’s disease. This movement disorder is characterised by the death of dopamine-producing nerve cells in a brainstem region called the substantia nigra (meaning “black substance”), named as such because it also contains cells that synthesise the skin pigment melanin. In brainstem tissue from Parkinson’s patients, pathological structures called Lewy bodies become visible under the microscope.
Banking on treatments and cures
We still have no cure for Parkinson’s disease, but there are treatments that can effectively alleviate its main symptoms. Most notably, approximately 200,000 Parkinson’s patients have been treated with an experimental surgical technique called deep brain stimulation (DBS). This involves implanting “brain pacemaker” electrodes into the brain, which can dramatically improve the tremor and muscle rigidity characteristic of the disease.

Donated brains are given an identification number and stored in a climate-controlled room awaiting dissection. The resulting samples are catalogued and neatly stacked, ready for future research and investigation.
With no effective treatments at present, Alzheimer’s disease remains a major public health issue whose prevalence in the Western world is predicted to increase significantly in the coming decades.
Having access to brain tissue from patients diagnosed with neurological diseases is crucial for researchers who study the conditions in the hope of advancing our understanding further, and for developing treatments and possibly even cures.
This is made possible by the people who donate their brains for scientific research. The research is facilitated by international “brain banks”, such as the UK Brain Banks Network, which stores post-mortem brain and central nervous system (CNS) tissue donated by the public for diagnosis and research into disorders. They will also provide advice and guidance if you are thinking of donating your brain after death.
Important neurological research is only possible because of the selfless generosity of donors. The devastating effects of neurological disease only add to the sense of awe neuroscientists feel when they examine the brain, and this makes them more determined to understand how it works and the many ways it can stop working properly.
You can watch a video of a pathological brain dissection on the Wellcome Collection YouTube channel. You have to be over 18 years of age to watch the video, in accordance with YouTube guidelines.
About the contributors
Moheb Costandi
Mo Costandi is a developmental neurobiologist turned freelance science writer. He is the author of three books: ‘Body Am I: The New Science of Self-Consciousness’ (MIT Press, 2022), ’Neuroplasticity’ (MIT Press, 2016) and ’50 Human Brain Ideas You Really Need to Know’ (Quercus, 2013).
Benjamin Gilbert
Ben is a senior photographer for Wellcome. He is happiest when telling stories with his photographs, whether that be the health implications of rural-to-urban migration in India, or the dedication of the workers who power the NHS.


